An HPV infection is a type of virus that frequently results in growths on the skin or mucous membranes (warts).
If you are hearing whispers about HPV all around you but are unsure about what it means, don’t worry; you are not alone. Many people have similar concerns. Human papillomavirus, or HPV, is a common illness that many people still find to be mysterious.
HPV is a dangerous virus that needs to be taken seriously. It is a common sexually transmitted infection that has been linked to several cancers in its hosts. The most direct type of cancer to be caused by HPV infection is cervical cancer, but other cancers of the mouth and throat as well as those of the anus, penis, vagina, and vulva can also be brought on by HPV infection.
This article aims to shed light on HPV, clearing up any misunderstandings and revealing the truth about this pervasive but mysterious virus.
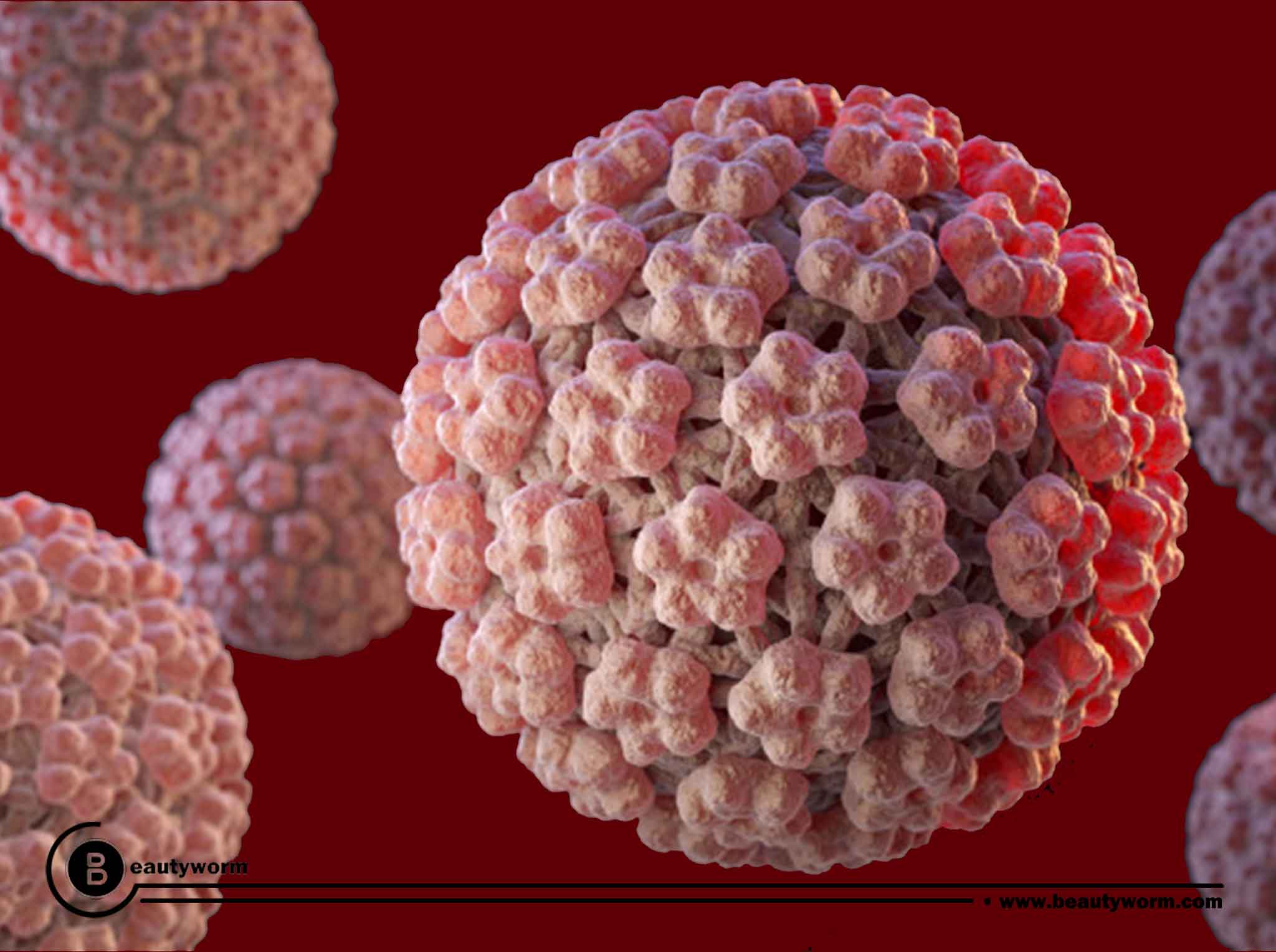
What is HPV?
Human papillomavirus (HPV) is a prevalent virus that has the potential to impact various areas of the body, potentially leading to a variety of health issues and complications if left untreated. Around hundred different strains of HPV exist, some of which can result in warts on the hands, feet, face, and other areas of the body. Your genitals, including your rectum and anus, as well as your vulva, vagina, cervix, penis, and scrotum, can be infected by any one of distinct HPV strains. This sexually transmitted infection (STI) affects your genitalia is spread by skin-to-skin contact. Though many people shudder at the mention of STIs, most strains of HPV in the genitalia are not harmful. This encompasses the variety of HPV that results in vaginal warts.
Cervical cancer is one of the diseases that some high-risk HPV strains can cause. Usually, early detection and treatment can prevent this.
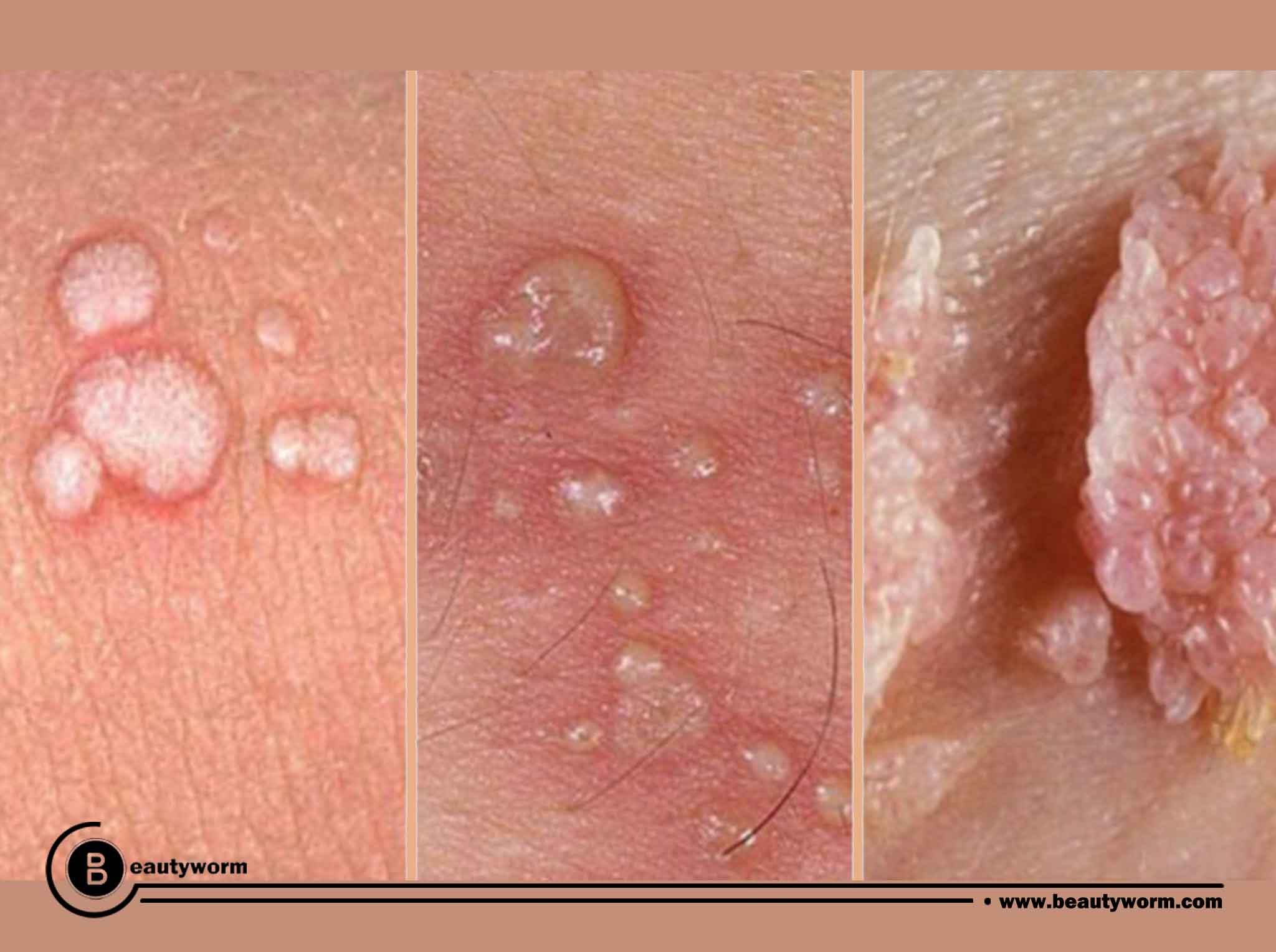
What are the symptoms of HPV?(The warts)
Before an HPV infection results in warts, your body’s immune system usually eradicates it. Depending on the type of HPV involved, warts can have a variety of appearances:
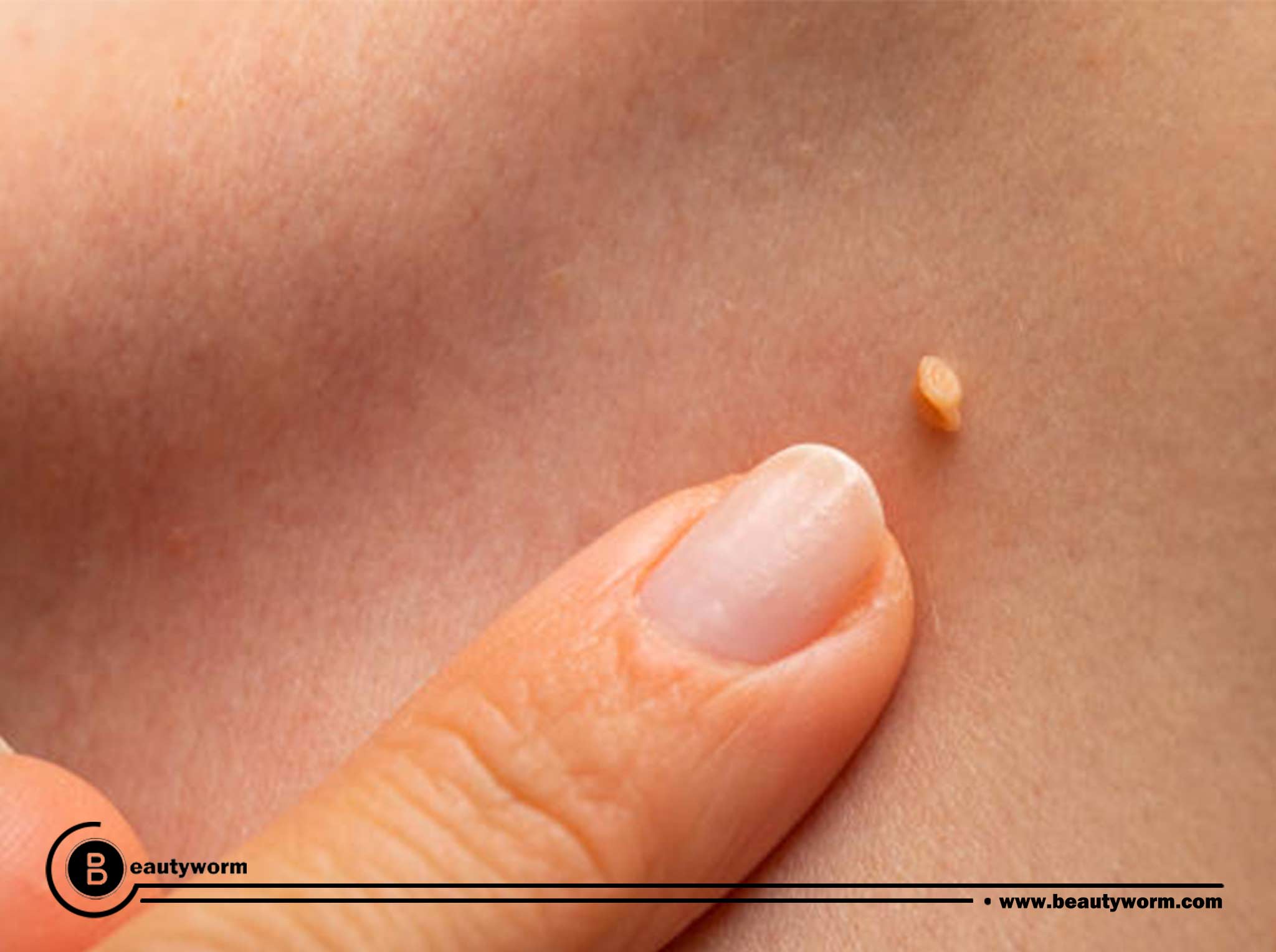
- Genital warts: Small cauliflower-like bumps, stem-like protrusions, or flat lesions are how this manifest. In females, vagina, the cervix, or the anus are the most common places for genital warts to emerge.
Genital warts in men typically develop around the anus, on the penis, and on the scrotum. Although they may itch or feel sensitive, genital warts rarely hurt or cause discomfort.
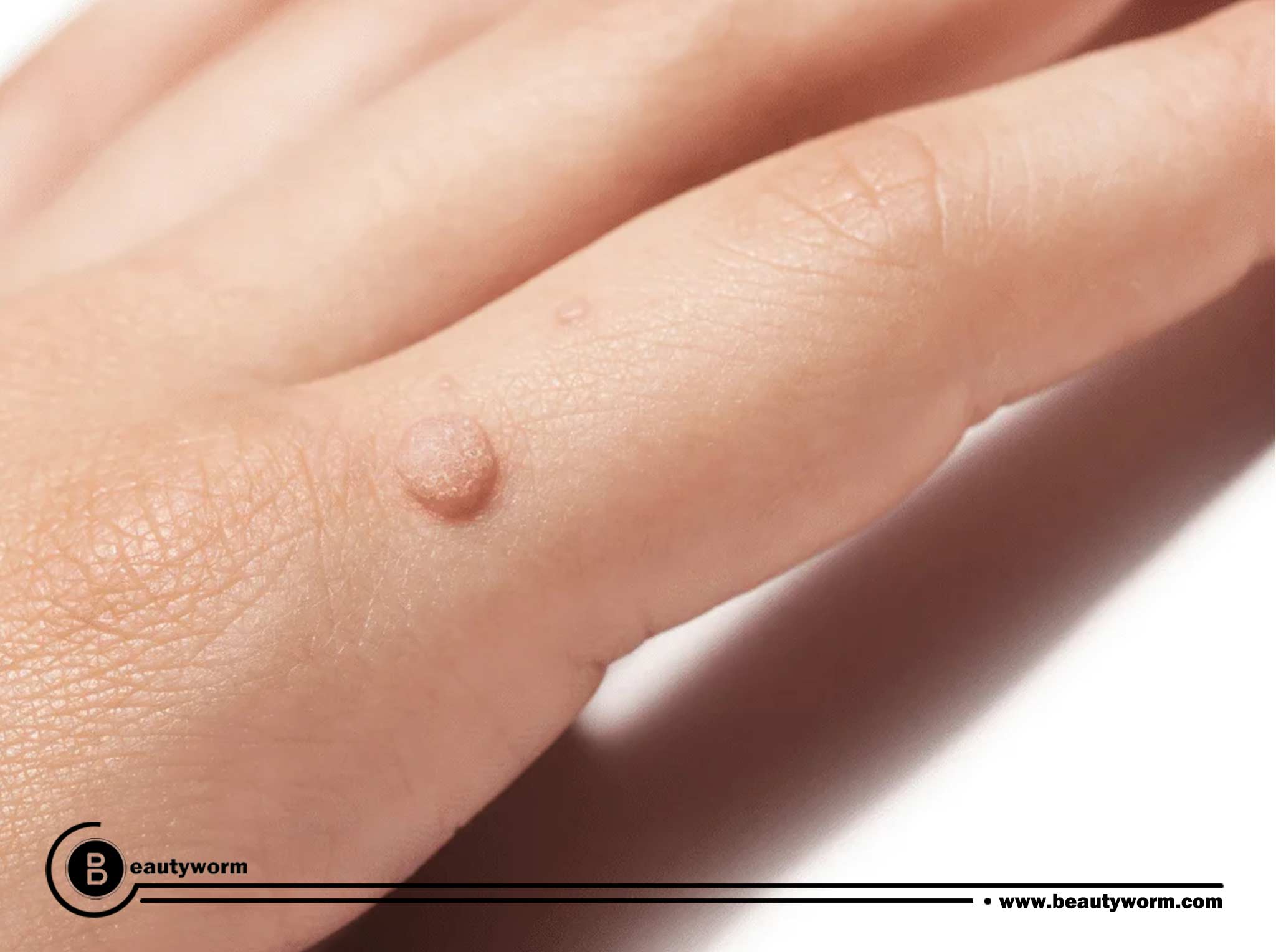
- Common warts: Usually located on the hands and fingers, common warts are rough, raised lumps. Common warts can hurt or be more prone to bleeding or injuries in addition to being unsightly most of the time.
- Plantar warts: Hard, granular growths called plantar warts typically develop on the balls or heels of the foot. These warts could be uncomfortable.
- Flat warts: Men usually experience these in their beard area, while children tend to have them more commonly on their face, such as cheeks, chin, and around the mouth area. However, they can appear anywhere. It usually affects women’s legs first.
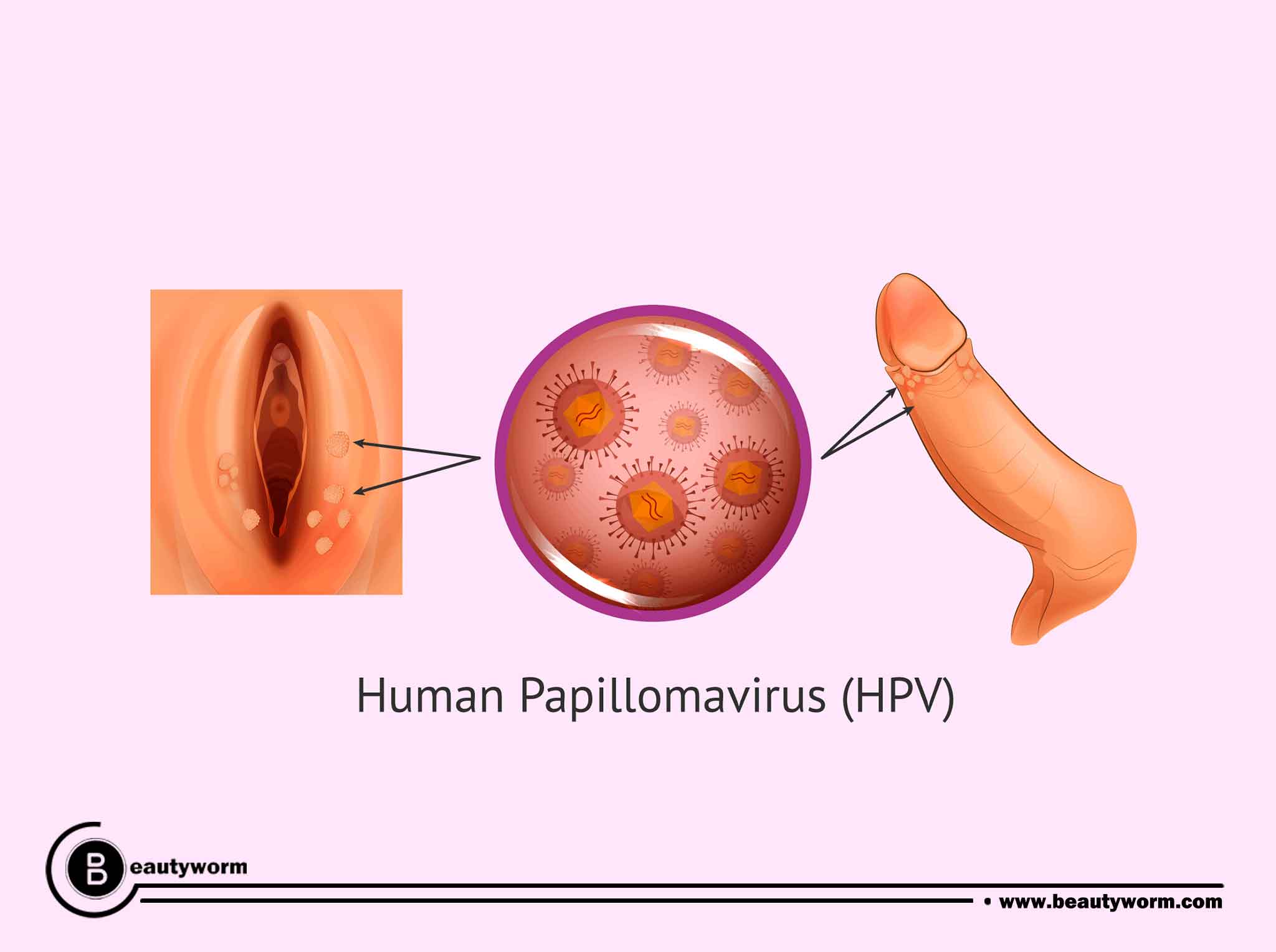
How is HPV spread?
Over the skin during intercourse, HPV is transferred from person to person. Around the whole genital area, the virus can reside on the skin. Shared sex toys or skin-to-skin genital contact are two common ways that it spreads from person to person during sexual contact. Although it doesn’t provide 100% protection, using a condom or other barrier contraception may lower your chance of contracting HPV.
All sexual orientations and those who have ever engaged in sexual activity are susceptible to HPV. This also applies if you:
- have partnered with one or more people sexually
- are linked to just one person for an extended period of time
Certain factors may increase your chance of continuing an HPV infection and developing cancer if you have a high-risk strain of the virus:
- an impaired defense mechanism
- possessing additional sexually transmitted infections, like chlamydia, herpes simplex, and gonorrhea
- protracted inflammation
- Cervical cancer caused by having numerous children
- long-term usage of oral contraceptives (cervical cancer)
- smoke products (cancer of the mouth or throat)
- having anal intercourse (anal cancer)
Our understanding of the transmission of HPV is incomplete. The virus can also spread through other channels, even though it is most commonly transmitted through sexual activity.
The virus may occasionally remain dormant in the body, according to another theory. This could continue for a few weeks, months, or even years following infection. This could indicate that years after you acquire it, it could become active once more.
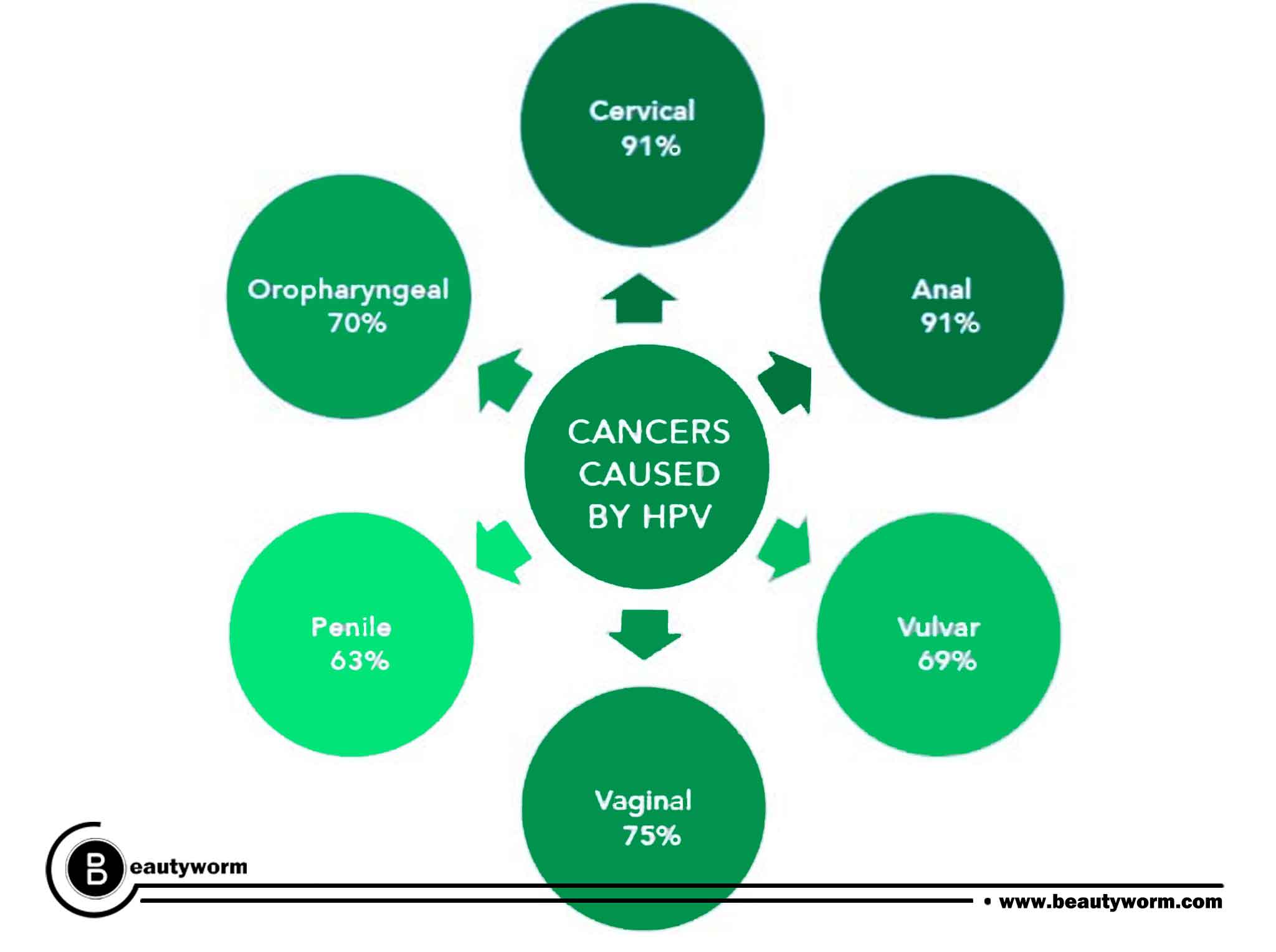
HPV and its relation to cancer
Cervical and other cancers, such as those of the vulva, vagina, penis, or anus, can be caused by HPV. Oropharyngeal cancer, a type of cancer that affects the back of the throat, can also result from it. This can apply to the tonsils and base of the tongue.
Most HPV infections go away on their own if you’re under 30. Your recommended testing frequency can be ascertained by age 30, if HPV is detected during a Pap smear (a test that screens for cervical cancer). Testing more frequently may be necessary if the results show that you are at a higher risk.
It is impossible to accurately anticipate which individuals may be affected by potentially life-threatening illnesses such as cancer and other health complications associated with HPV infections. HPV may be harder for those with weakened immune systems to fight off, including those living with HIV. Additionally, there may be a higher chance of HPV-related health issues.
How does HPV affect Women?
Over the course of their lives, 80 percent of women are expected to get at least one form of HPV. Similar to men, the majority of women infected with HPV do not show any symptoms, and the infection resolves on its own without worsening their health.
Genital warts can appear inside the vagina, in or around the anus, on the cervix or vulva, and some women may become aware that they have them.
If you observe any lumps or growths in or near your genital area that seem strange, schedule a visit with your doctor.
Certain HPV strains can result in cancers of the vagina, anus, or throat in addition to cervical cancer. Women who undergo routine screening can be helped to identify the changes linked to cervical cancer. Furthermore, HPV strains linked to genital cancers can be identified through DNA testing on cervical cells.

How does HPV affect Men?
While some men who get HPV infection may get genital warts, the majority of men do not exhibit any symptoms. If you observe any unusual lumps or lesions on your scrotum, anus, or penis, consult a physician.
Men who have certain HPV strains may develop throat, anal, or penile cancer. Men who have weaker immune systems or who engage in anal intercourse may be more vulnerable to HPV-related cancers.
The HPV strains responsible for genital warts are distinct from those that cause cancer.

What are the causes and risk factors of HPV?
A cut, scrape, or tear in your skin allows the human papillomavirus to enter your body and infect you. It is contracted through oral, anal, or vaginal sex as well as skin-to-skin contact. If you have genital warts while you’re pregnant, you could transmit HPV to your unborn child. a noncancerous growth in your baby’s voice box (larynx) may result from this in rare instances.
The warts can easily spread from person to person due to their contagious nature. They can be contracted by touching a surface that has come into contact with a wart or by touching someone else’s wart.
There are certain factors that increase your risk of HPV. Among them are:
- Damaged skin: Common warts tend to appear more frequently on areas of your skin with holes or frequent cuts.
- Direct contact: HPV can infect you if you come into contact with someone who has a wart on their body or if you touch a wart-ridden surface.
- Number of sexual partners: You have a higher chance of contracting HPV if you have multiple sexual partners. Additionally, your risk is increased if you have sex with someone who has multiple partners.
- Age: Common warts are more likely to affect children. Teenagers and early adults are more likely to develop vaginal warts.
- Weak immune system: You are more susceptible to HPV if you have an immune-suppressive medication or an underlying medical condition like HIV or AIDS.
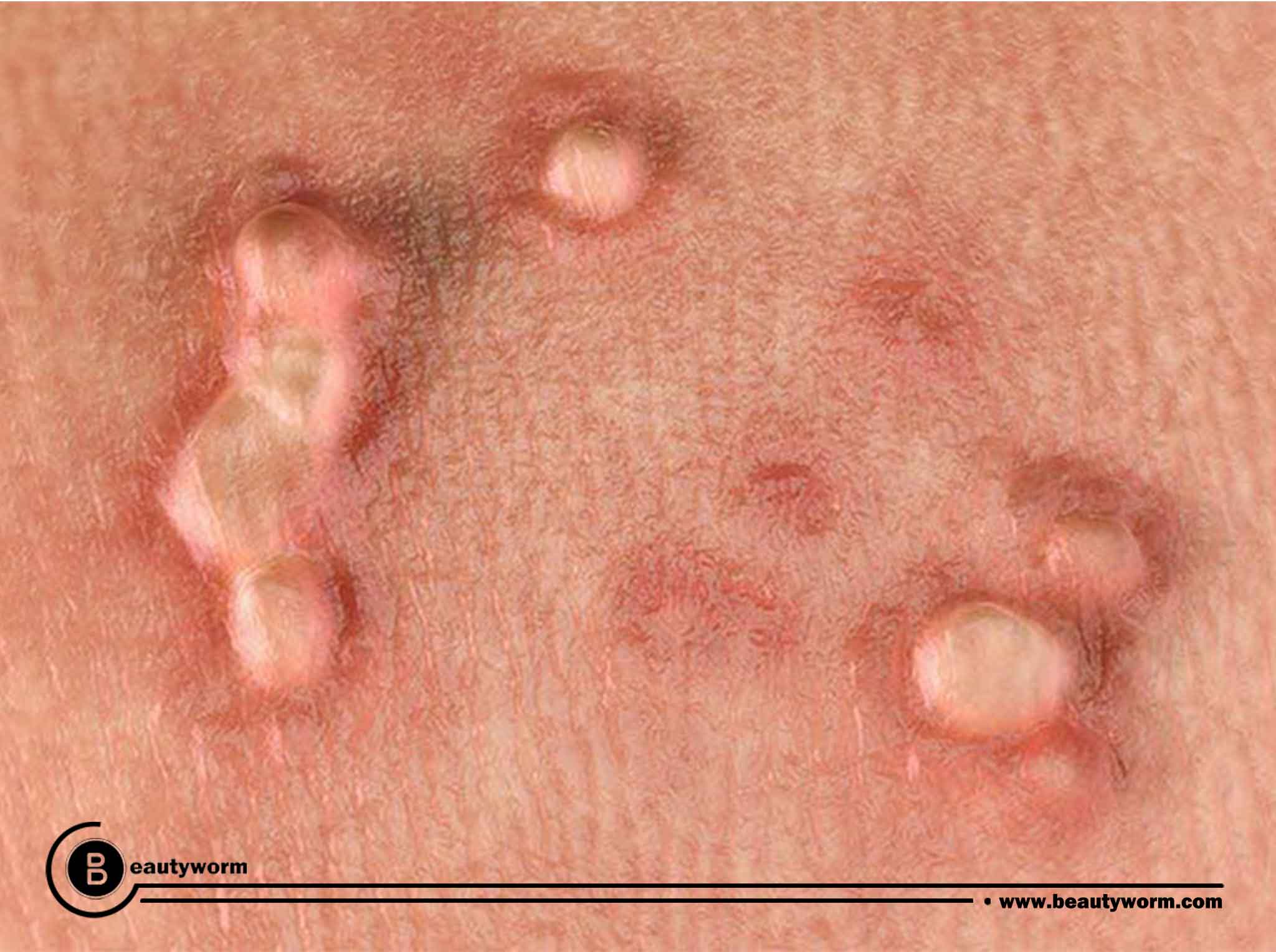
Can HPV be dormant? How long?
It is important to note that the human papillomavirus (HPV) has the ability to remain inactive in the body for a significant amount of time following initial infection, potentially spanning several years, without presenting any noticeable symptoms.
The immune system battles and gets rid of the virus from the body in one to two years in the majority of HPV cases. Once that happens, the virus vanishes and becomes incapable of spreading to new hosts.
When conditions are dire, HPV can lie dormant in the body for many years. Even in the absence of symptoms, the virus can still spread during this period since it is constantly replicating inside of cells.
This is also the reason why HPV can test positive even after years of dormancy. It can spread from one partner to all partners for up to ten years, so getting tested is essential.
What is HPV vaccine and Who should get it?
A key strategy in lowering the number of people with high-risk HPV and, consequently, the number of cases of HPV-related cancers, is HPV vaccination. The HPV vaccine is made available to all children in the UK between the ages of 12 and 13.
Vaccines don’t aim to treat infections that already exist; instead, they aim to lower the risk of contracting an infection. Due to the fact that they are probably not yet exposed to HPV, the vaccination program includes children of this age, which improves its effectiveness. The HPV vaccine loses some of its efficacy after a person has been exposed.
If you weren’t vaccinated when it was offered at school, you can request one for free up until the age of 25. Through sexual health clinics, men who have sex with men up to 45 years old can also receive the vaccine. If you don’t fit these requirements, you can pay for a private vaccination, but if you have already been exposed to the virus—which most of us have been as adults—the shot might not work.
Maintaining a routine cervical screening schedule is the best defense against cervical cancer. Even if you have received the HPV vaccine, it is still important to undergo cervical screening as the vaccine may not provide complete protection against HPV.
What are the possible HPV vaccine side effects?
As with all medications, side effects are possible with vaccines. A day or two is all that is needed for the mild side effects of HPV shots to subside. these include:
- edema, pain, or redness in the arm from the injection site
- Fever
- dizziness or fainting (teenagers are more likely than adults to faint following any vaccination, including the HPV vaccine)
- Nausea
- Headache or fatigue
- Muscle or joint pain
Teens should remain seated or lie down during the vaccination and for fifteen minutes following the administration in order to minimize fainting and injuries resulting from it.
Any severe allergies your child may have, such as a latex or yeast allergy, should be reported to the doctor or nurse.
What are the HPV tests?
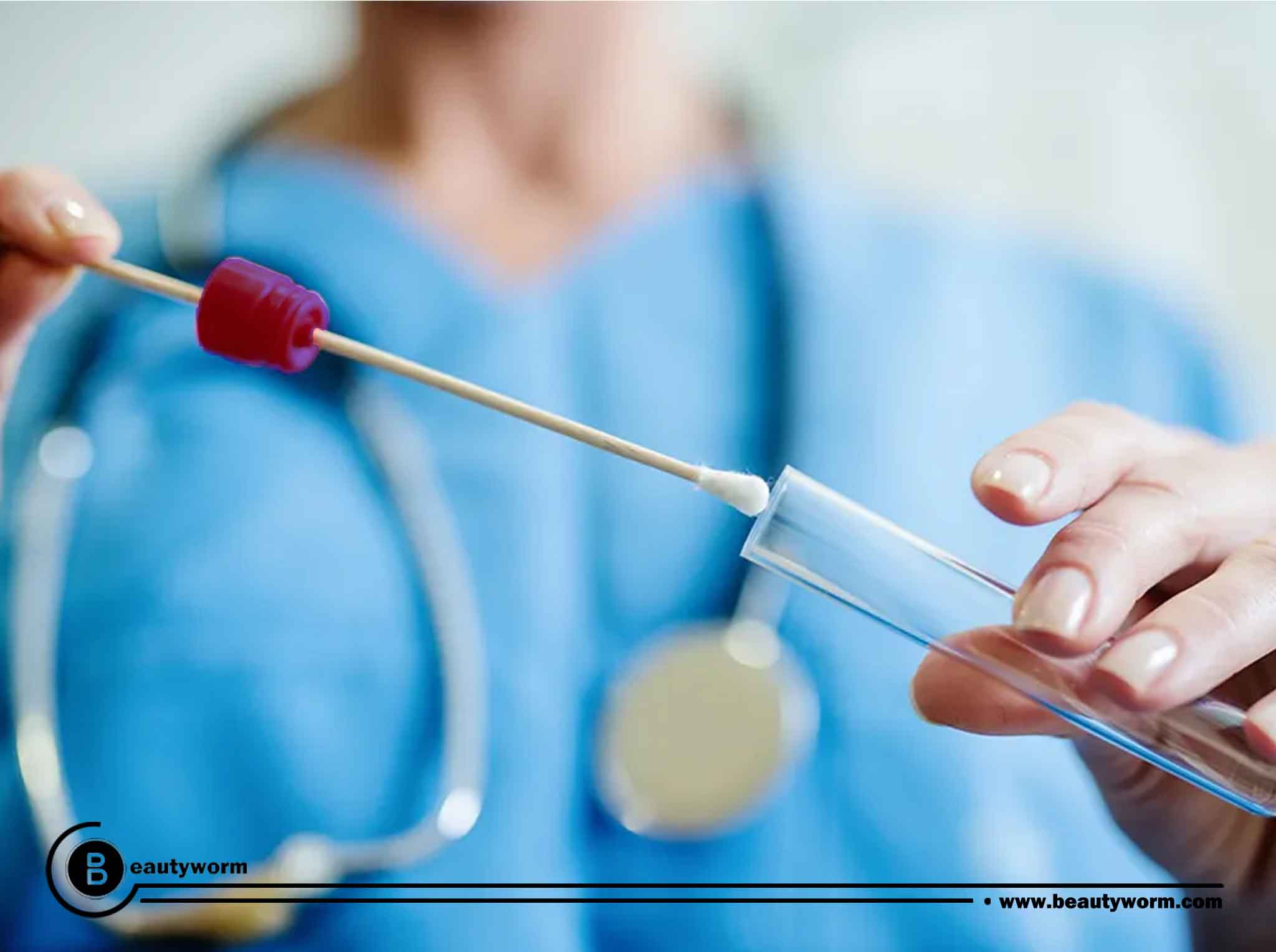
HPV testing is an integral component of cervical screening procedures, which play a crucial role in detecting potential health risks early on. It is important to note that unlike some other tests, there isn’t a specific blood test available for HPV detection.
An HPV test is performed on a tiny sample of cervix cells during cervical screening. Following certain procedures, abnormal cells most likely caused by an HPV infection can be found:
- Pap smear: A Pap smear checks for precancerous cells that, if left untreated, can develop into cervical dysplasia, a cancer. Most often, high-risk HPV is the cause of cervical cancer.
- HPV test: Tests for HPV can identify high-risk virus strains that, if untreated, could cause cervical cancer. As far as testing for HPV on the vulva, vagina, penis, scrotum, rectum, or anus is concerned, there are none that have received U.S. Food and Drug Administration (FDA) approval. HPV-related malignancies on various body areas are significantly less common than cervical cancer.
- Colposcopy: If your Pap smear reveals abnormal cells or if you tested positive for HPV, your doctor might prescribe a colposcopy. Abnormal cells are visible on your cervix thanks to a bright device called a colposcope, which is used during this process. Your doctor might take the cells out and have a lab test done to see if there are any indications of cancer or precancerous growths.
- Visual inspection with acetic acid (VIA): In areas where resources for routine HPV testing or Pap smears are unavailable, providers may choose to employ VIA. Your doctor applies a vinegar-based solution to your cervix when using VIA. The solution makes aberrant cells white, making them more noticeable.
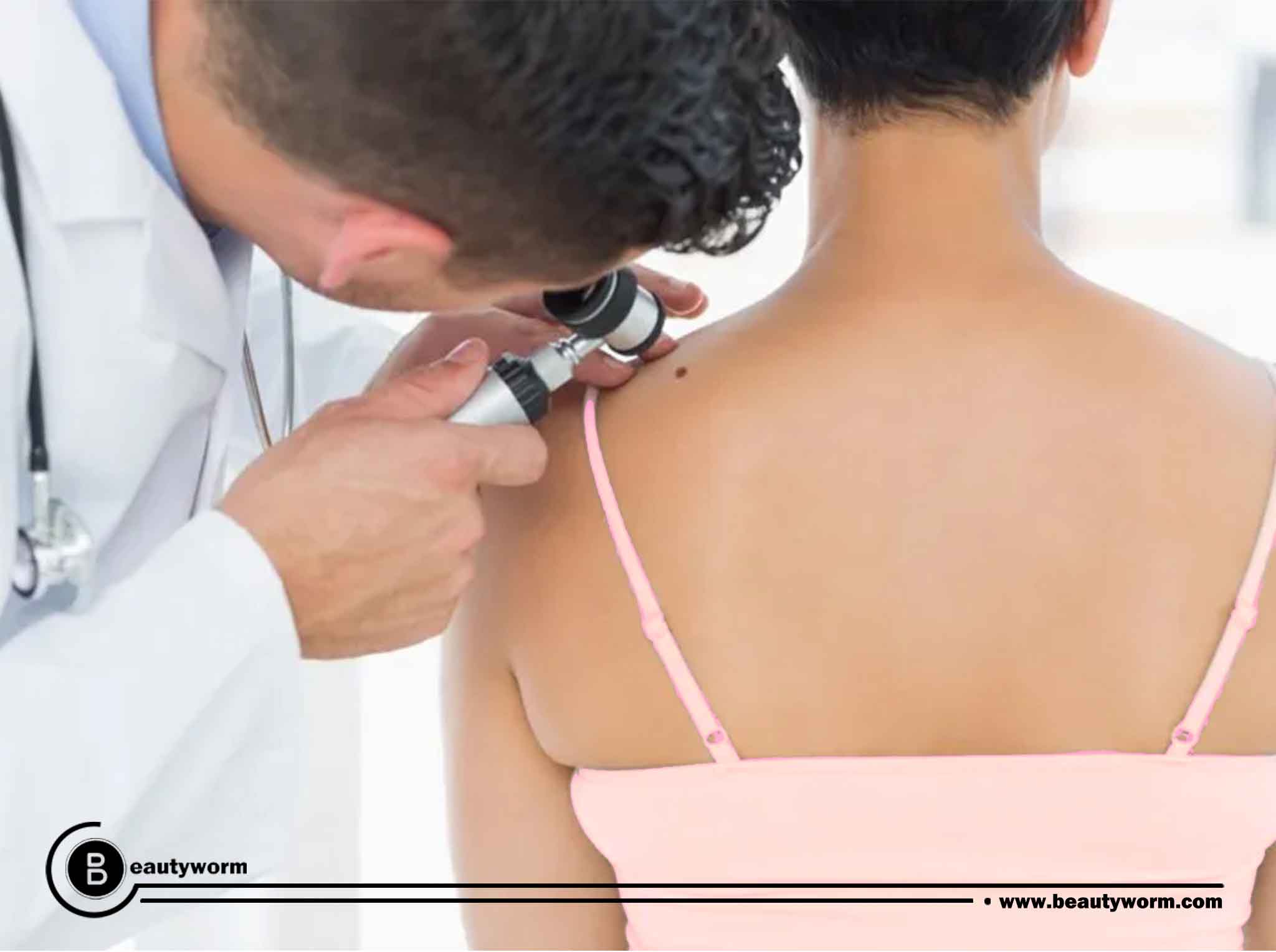
What are the treatments of HPV?
Treatments cannot eradicate the virus from your body. However, they can remove any visible genital warts from your cervix as well as any abnormal cells within it. Treatment options could be:
- Cryosurgery: applying liquid nitrogen to warts to destroy abnormal cells.
- Loop electrosurgical excision procedure (LEEP): The cervix, which is the opening between the uterus and vagina, is treated medically with this procedure to remove abnormal cells.
- Electrocautery: using an electrical current to burn off warts.
- Laser therapy: eliminating warts and any aberrant cells with a strong light.
- Cold knife cone biopsy (conization): removal of a cervical tissue fragment in the form of a cone that contains aberrant cells.
- Prescription cream: To eradicate warts, apply medicated cream directly to the affected area. Both podofilox and imiquimod may be present in these creams.
- Trichloroacetic acid (TCA): applying a wart-burning chemical treatment.
Treatment-requiring abnormal cervical cells only occur in a small percentage of high-risk HPV infections.

Prevention of HPV
Using condoms and having safe sexual practices are the most straightforward ways to prevent HPV.
Moreover, HPV-related cancers and genital warts can be avoided with the Gardasil 9 vaccination. Nine HPV strains that are known to be connected to either genital warts or cancer can be prevented by the vaccine.
For boys and girls ages 11 or 12, the CDC advises getting the HPV vaccine. There is a minimum of six months gap between the two vaccination doses. Also eligible for vaccination on a three-dose schedule are men and women between the ages of 15 and 26.
Moreover, individuals aged between 27 and 45 who have not received a prior HPV vaccination are now eligible to receive the Gardasil 9 vaccine.
A Pap smear, screening, and regular check-ups are important ways to avoid health issues related to HPV.
FAQs
In this part, let’s take a look at a few commonly asked questions by the users.
Can I give HPV to my kids?
It is unlikely that you could transmit HPV to your children unless you have genital skin-to-skin contact with them, as sexual contact is the primary way in which it is spread.
If I’ve had HPV once, can I get it again?
After your body eliminates the HPV strain, you cannot contract it again. It is possible to come into contact with a different strain of HPV, though, as there are more than 100 varieties.
Can I live a normal life with HPV?
Yes, without a doubt! It's crucial to keep in mind that having HPV does not have to significantly interfere with your everyday activities or prevent you from going about your daily business.
What vitamins clear up HPV faster?
There isn't any scientific proof as of yet that certain vitamins can eradicate HPV directly. A healthy lifestyle that boosts your immune system, however, can be advantageous.
Is HPV very serious?
HPV is extremely common and frequently harmless, despite the fact that it can occasionally be dangerous. Reducing your risk of developing HPV-related health problems can be achieved by receiving the vaccine, practicing safe sexual practices, and regularly scheduling checkups.
Summary
The HPV virus can spread silently and without showing any symptoms because it can remain dormant in the body for extended periods of time. It is imperative to routinely get tested for sexually transmitted infections (STIs) in order to stop the spread of these infections. When a new partner enters your life or if any of your partners have extramarital affairs, it is strongly advised that you arrange for STI screenings.
Knowing whether you have HPV plays a vital role in preventing complications and preventing the virus from spreading to others, which improves public health and wellbeing in general.
References: Ref1 Ref2 Ref3 Ref4 Ref5 Ref6 Ref7 Ref8 Ref9 Ref10 Ref11 Ref12









Using herbal natural remedy was what got me tested negative to HPV 2 after been diagnosed for years.I have spend so much funds on medications like acyclovir (Zovirax), Famciclovir (Famvir), and Valacyclovir (Valtrex). But it was all a waste of time and my symptoms got worse. To me It is very bad what Big pharma are doing, why keep making humans suffer greatly just to get profits annually for medications that don’t work. I’m glad that herbal remedies are gaining so much awareness and many people are getting off medications and activating their entire body system with natural herbal remedies and they have become holistically healed totally.